Typhoid fever
| Typhoid fever | |
|---|---|
| Classification and external resources | |
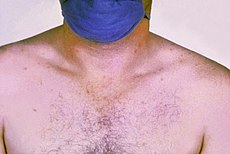
Rose spots on the chest of a patient with typhoid fever due to the bacterium SalmonellaTyphi
| |
Typhoid fever — also known simply as typhoid[1] — is a common worldwide bacterial disease transmitted by the ingestion of food or water contaminated with the feces of an infected person, which contain the bacterium Salmonella enterica enterica, serovar Typhi.[2]
The disease has received various names, such as gastric fever, enteric fever, abdominal typhus, infantile remittant fever,slow fever, nervous fever and pythogenic fever. The name typhoid means "resembling typhus" and comes from the neuropsychiatric symptoms common to typhoid and typhus.[3] Despite this similarity of their names, typhoid fever and typhus are distinct diseases and are caused by different species of bacteria.[4]
The occurrence of this disease fell sharply in the developed world with the rise of 20th-century sanitation techniques andantibiotics
Signs and symptoms
Classically, the course of untreated typhoid fever is divided into four individual stages, each lasting approximately one week. Over the course of these stages, the patient becomes exhausted and emaciated.[7]
- In the first week, the temperature rises slowly, and fever fluctuations are seen with relative bradycardia (Faget sign), malaise, headache, and cough. A bloody nose (epistaxis) is seen in a quarter of cases, and abdominal pain is also possible. There is a decrease in the number of circulating white blood cells (leukopenia) with eosinopenia and relative lymphocytosis; blood cultures are positive for Salmonella typhi or paratyphi. The Widal test is negative in the first week.[citation needed]
- In the second week of the infection, the patient lies prostrate with high fever in plateau around 40 °C (104 °F) and bradycardia (sphygmothermic dissociation or Faget sign), classically with a dicrotic pulse wave. Delirium is frequent, often calm, but sometimes agitated. This delirium gives to typhoid the nickname of "nervous fever". Rose spotsappear on the lower chest and abdomen in around a third of patients. There are rhonchi in lung bases.
- The abdomen is distended and painful in the right lower quadrant, where borborygmi can be heard. Diarrhea can occur in this stage: six to eight stools in a day, green, comparable to pea soup, with a characteristic smell. However, constipation is also frequent. The spleen and liver are enlarged (hepatosplenomegaly) and tender, and there is elevation of liver transaminases. The Widal test is strongly positive, with antiO and antiH antibodies. Blood cultures are sometimes still positive at this stage.
- (The major symptom of this fever is that the fever usually rises in the afternoon up to the first and second week.)
- In the third week of typhoid fever, a number of complications can occur:
- Intestinal haemorrhage due to bleeding in congested Peyer's patches; this can be very serious but is usually not fatal.
- Intestinal perforation in the distal ileum: this is a very serious complication and is frequently fatal. It may occur without alarming symptoms until septicaemia or diffuseperitonitis sets in.
- Encephalitis
- Neuropsychiatric symptoms (described as "muttering delirium" or "coma vigil"), with picking at bedclothes or imaginary objects.
- Metastatic abscesses, cholecystitis, endocarditis and osteitis
- The fever is still very high and oscillates very little over 24 hours. Dehydration ensues, and the patient is delirious (typhoid state). One third of affected individuals develop a macular rash on the trunk.
- Platelet count goes down slowly and risk of bleeding rises.
- By the end of third week, the fever starts subsiding (defervescence). This carries on into the fourth and final week.
Transmission
The bacterium that causes typhoid fever may be spread through poor hygiene habits and public sanitation conditions, and sometimes also by flying insects feeding on feces. Public education campaigns encouraging people to wash their hands after defecating and before handling food are an important component in controlling spread of the disease. According to statistics from the United States Centers for Disease Control and Prevention (CDC), the chlorination of drinking water has led to dramatic decreases in the transmission of typhoid fever in the U.S.A.
Diagnosis
Diagnosis is made by any blood, bone marrow or stool cultures and with the Widal test (demonstration of salmonella antibodies against antigens O-somatic and H-flagellar). In epidemics and less wealthy countries, after excluding malaria, dysentery or pneumonia, a therapeutic trial time with chloramphenicol is generally undertaken while awaiting the results of the Widal test and cultures of the blood and stool.[8]
The Widal test is time-consuming, and often, when a diagnosis is reached, it is too late to start an antibiotic regimen.
The term enteric fever is a collective term that refers to severe typhoid and paratyphoid.[9]
Prevention
Main article: Typhoid vaccine
Sanitation and hygiene are the critical measures that can be taken to prevent typhoid. Typhoid does not affect animals, and therefore, transmission is only from human to human. Typhoid can only spread in environments where human feces or urine are able to come into contact with food or drinking water. Careful food preparation and washing of hands are crucial to prevent typhoid.
There are two vaccines licensed for use for the prevention of typhoid:[10] the live, oral Ty21a vaccine (sold as Vivotif by Crucell Switzerland AG) and the injectable Typhoid polysaccharide vaccine (sold as Typhim Vi by Sanofi Pasteur and Typherix by GlaxoSmithKline). Both are 50% to 80% protective and are recommended for travellers to areas where typhoid is endemic. Boosters are recommended every five years for the oral vaccine and every two years for the injectable form. There exists an older, killed-whole-cell vaccine that is still used in countries where the newer preparations are not available, but this vaccine is no longer recommended for use because it has a higher rate of side effects (mainly pain and inflammation at the site of the injection).[10]
Treatment
The rediscovery of oral rehydration therapy in the 1960s provided a simple way to prevent many of the deaths of diarrheal diseases in general.
Where resistance is uncommon, the treatment of choice is a fluoroquinolone such as ciprofloxacin.[9][11] Otherwise, a third-generation cephalosporin such as ceftriaxone or cefotaxime is the first choice.[12][13][14] Cefixime is a suitable oral alternative.[15][16]
Typhoid fever, when properly treated, is not fatal in most cases. Antibiotics, such as ampicillin, chloramphenicol, trimethoprim-sulfamethoxazole, amoxicillin and ciprofloxacin, have been commonly used to treat typhoid fever in microbiology (Baron S et al.). Treatment of the disease with antibiotics reduces the case-fatality rate to approximately 1%.[17]
When untreated, typhoid fever persists for three weeks to a month. Death occurs in between 10% and 30% of untreated cases.[18] In some communities, however, case-fatality rates may reach as high as 47%.[citation needed]
Surgery
Surgery is usually indicated in cases of intestinal perforation. Most surgeons prefer simple closure of the perforation with drainage of the peritoneum. Small-bowel resection is indicated for patients with multiple perforations.
If antibiotic treatment fails to eradicate the hepatobiliary carriage, the gallbladder should be resected. Cholecystectomy is not always successful in eradicating the carrier state because of persisting hepatic infection.
Resistance
Resistance to ampicillin, chloramphenicol, trimethoprim-sulfamethoxazole, and streptomycin is now common, and these agents have not been used as first–line treatment for almost twenty years.[citation needed] Typhoid that is resistant to these agents is known as multidrug-resistant typhoid (MDR typhoid).
Ciprofloxacin resistance is an increasing problem, especially in the Indian subcontinent and Southeast Asia. Many centres are therefore moving away from using ciprofloxacin as the first line for treating suspected typhoid originating in South America, India, Pakistan, Bangladesh, Thailand, or Vietnam. For these patients, the recommended first line treatment is ceftriaxone. It has also been suggested that azithromycin is better at treating typhoid in resistant populations than both fluoroquinolone drugs and ceftriaxone.[11]Azithromycin significantly reduces relapse rates compared with ceftriaxone.
There is a separate problem with laboratory testing for reduced susceptibility to ciprofloxacin: current recommendations are that isolates should be tested simultaneously against ciprofloxacin (CIP) and against nalidixic acid (NAL), and that isolates that are sensitive to both CIP and NAL should be reported as "sensitive to ciprofloxacin", but that isolates testing sensitive to CIP but not to NAL should be reported as "reduced sensitivity to ciprofloxacin". However, an analysis of 271 isolates showed that around 18% of isolates with a reduced susceptibility to ciprofloxacin (MIC 0.125–1.0 mg/l) would not be picked up by this method.[19] It is not certain how this problem can be solved, because most laboratories around the world (including the West) are dependent on disk testing and cannot test for MICs.
Epidemiology
In 2000, typhoid fever caused an estimated 21.7 million illnesses and 217,000 deaths.[20] Its incidence is highest in children and young adults between 5 and 19 years old.[18] These cases as of 2010 caused about 190,000 deaths up from 137,000 in 1990.[21] Infants, children, and adolescents in south-central and Southeastern Asia experience the greatest burden of illness.[22] Nonetheless, outbreaks of typhoid fever are frequently reported from sub-Saharan Africa and countries in Southeastern Asia.[23][24] Historically, in the pre-antibiotic era, the case fatality rate of typhoid fever was 10–20%. Today, with prompt treatment, it is less than 1%.[25] However, about 3-5% of individual who are infected will develop a chronic infection in the gall bladder.[26] Since Typhi is human-restricted, these chronic carriers become the crucial reservoir and can persist for decades for further spread of the disease, further complicates the identification and treatment of the disease.[27] Lately, the study of Typhi associated with a carrier at the genome level provides new insights into the pathogenesis of the pathogen.[28]
History
Around 430–424 BC, a devastating plague, which some believe to have been typhoid fever, killed one third of the population of Athens, including their leader Pericles. The balance of power shifted from Athens to Sparta, ending the Golden Age of Pericles that had marked Athenian dominance in the Greek ancient world. The ancient historianThucydides also contracted the disease, but he survived to write about the plague. His writings are the primary source on this outbreak and modern academics and medical scientists consider epidemic typhus the most likely cause. In 2006 a study detected DNA sequences similar to those of the bacterium responsible for typhoid fever in dental pulpextracted from a burial pit dated to the time of the outbreak.[29]
The cause of the plague has long been disputed and other scientists have disputed the findings, citing serious methodologic flaws in the dental pulp-derived DNA study.[30] The disease is most commonly transmitted through poor hygiene habits and public sanitation conditions; during the period in question, the whole population of Attica was besieged within the Long Walls and lived in tents.
Some historians believe that the English colony of Jamestown, Virginia, died out from typhoid. Typhoid fever killed more than 6000 settlers between 1607 and 1624.[31]
During the American Civil War, 81,360 Union soldiers died of typhoid or dysentery.[32] In the late 19th century, the typhoid fever mortality rate in Chicago averaged 65 per 100,000 people a year. The worst year was 1891, when the typhoid death rate was 174 per 100,000 people.[33]
The most notorious carrier of typhoid fever—but by no means the most destructive—was Mary Mallon, also known as Typhoid Mary. In 1907, she became the first American carrier to be identified and traced. She was a cook in New York. She is closely associated with fifty-three cases and three deaths.[34] Public health authorities told Mary to give up working as a cook or have her gall bladder removed. Mary quit her job but returned later under a false name. She was detained and quarantined after another typhoid outbreak. She died of pneumonia after 26 years in quarantine.
Development of vaccination
During the course of treatment of a typhoid outbreak in a local village in 1838, English country doctor William Budd realised that the "poisons" involved in infectious diseasesmultiplied in the intestines of the sick, were present in their excretions, and could then be transmitted to the healthy through their consumption of contaminated water.[35] He proposed strict isolation as a method for containing such outbreaks in the future.[36] The medical and scientific communities did not identify the role of microorganisms in infectious disease until the work of Louis Pasteur.
In 1880 Karl Joseph Eberth described a bacillus that he suspected was the cause of typhoid. In 1884 pathologist Georg Theodor August Gaffky (1850–1918) confirmed Eberth's findings, and the organism was given names such as Eberth's bacillus, Eberthella typhi and Gaffky-Eberth bacillus. Today the bacillus that causes typhoid fever goes by the scientific name of Salmonella enterica enterica, serovar Typhi.
The British bacteriologist Almroth Edward Wright first developed an effective typhoid vaccine at the Army Medical School in Netley,Hampshire. It was introduced in 1896 and used successfully during the Boer War.[37] At that time typhoid often killed more soldiers at war than were lost due to enemy combat. He further developed his vaccine at a newly opened research department at St Mary's HospitalMedical School in London from 1902, where he established a method for measuring protective substances (opsonin) in human blood.
Citing the example of the Second Boer War, during which many soldiers died from easily preventable diseases, Wright convinced theBritish Army that 10 million vaccines should be produced for the troops being sent to the Western Front, thereby saving up to half a million lives during the War.[38] The British Army was the only combatant at the outbreak of the war to be fully immunized against the bacteria, which meant that for the first time, casualties due to combat exceeded those from disease.[10]
In 1909, Frederick F. Russell, a U.S. Army physician, adopted Wright's typhoid vaccine for use with the US Army and two years later his vaccination program became the first in which an entire army was immunized. It eliminated typhoid as a significant cause of morbidity and mortality in the U.S. military.[39]
Most developed countries saw declining rates of typhoid fever throughout the first half of the 20th century due to vaccinations and advances in public sanitation and hygiene. In 1908, the chlorination of drinking water was a significant step in the control of typhoid fever in the U.S. The first permanent disinfection of drinking water in the U.S. occurred on the Jersey City, New Jersey water supply. Credit for the decision to build the chlorination system has been given to John L. Leal[40] The chlorination facility was designed by George W. Fuller.[41]Antibiotics were introduced in clinical practice in 1942, greatly reducing mortality. Today, the incidence of typhoid fever in developed countries is around 5 cases per 1,000,000 people per year.
A notable outbreak occurred in Aberdeen, Scotland in 1964. This was due to contaminated tinned meat sold at the city's branch of theWilliam Low chain of stores. No fatalities resulted.
An outbreak in the Democratic Republic of Congo in 2004–05 recorded more than 42,000 cases and 214 deaths.[18]
Notable cases
- Roger Sherman, one of the Founding Fathers of the United States died of typhoid fever in 1793.
- Gerard Manley Hopkins, English poet, died of typhoid fever in 1889.[42]
- Prince Albert, husband of Queen Victoria, died of typhoid fever at the age of 42.
- Major Gonville Bromhead, who fought in the Battle of Rorke's Drift, depicted in the film Zulu, died of typhoid fever in India in 1891.
- Dr HJH 'Tup' Scott, captain of the 1886 Australian cricket team that toured England, died of typhoid in 1910.[43]
- Wilbur Wright, the older of the two Wright Brothers, died of typhoid on May 30, 1912.
- Edith Claypole, a British scientist, died of typhoid in 1915. She acquired the disease while preparing vaccinations for WWI troops, despite the protection of having been vaccinated herself.
- Arnold Bennett, English novelist, died in 1932 of typhoid, two months after drinking a glass of water in a Paris hotel to prove it was safe.[44]
- Hakaru Hashimoto, Japanese medical scientist, died of typhoid fever in 1934.[45]
- Mary Mallon, a.k.a. "Typhoid Mary", presumed to have infected 51 people over her career as a cook, died 1938.
- Heath Bell, a relief pitcher for the San Diego Padres acquired typhoid on a 2010 trip to Fiji but survived.[46]
- Louisa May Alcott, author of Little Women acquired typhoid while being a nurse at a hospital in Washington, D.C. but survived.







.jpg)
.jpg)
.jpg)
.jpg)



No comments:
Post a Comment